If you open any social media app or news site, chances are the first thing…
What it’s like to work as a nurse in NYC during the Coronavirus Pandemic
an interview with healthcare professional Angélica Ortiz21 April 2020
We at YEOJA Mag are determined to continue to bring you our regular content but have also decided as a team to feature certain articles pertaining to COVID-19 as it impacts our community, from mental health, to xenophobia. You can find all COVID-19-related pieces here. There will be a lot to unpack and discuss in the coming weeks and months. But firstly, we want to help alleviate some of the stress that a lot of people are feeling and talk about mental health in times of social distancing, self isolation, and quarantine.
The spread of COVID-19 has impacted the entire world on in unprecedented ways. The United States currently has the highest number of confirmed cases and deaths. Within its borders, New York has been hit the hardest, with 242.786 confirmed cases and 13.869 deaths, 10.022 of them in New York City alone.*
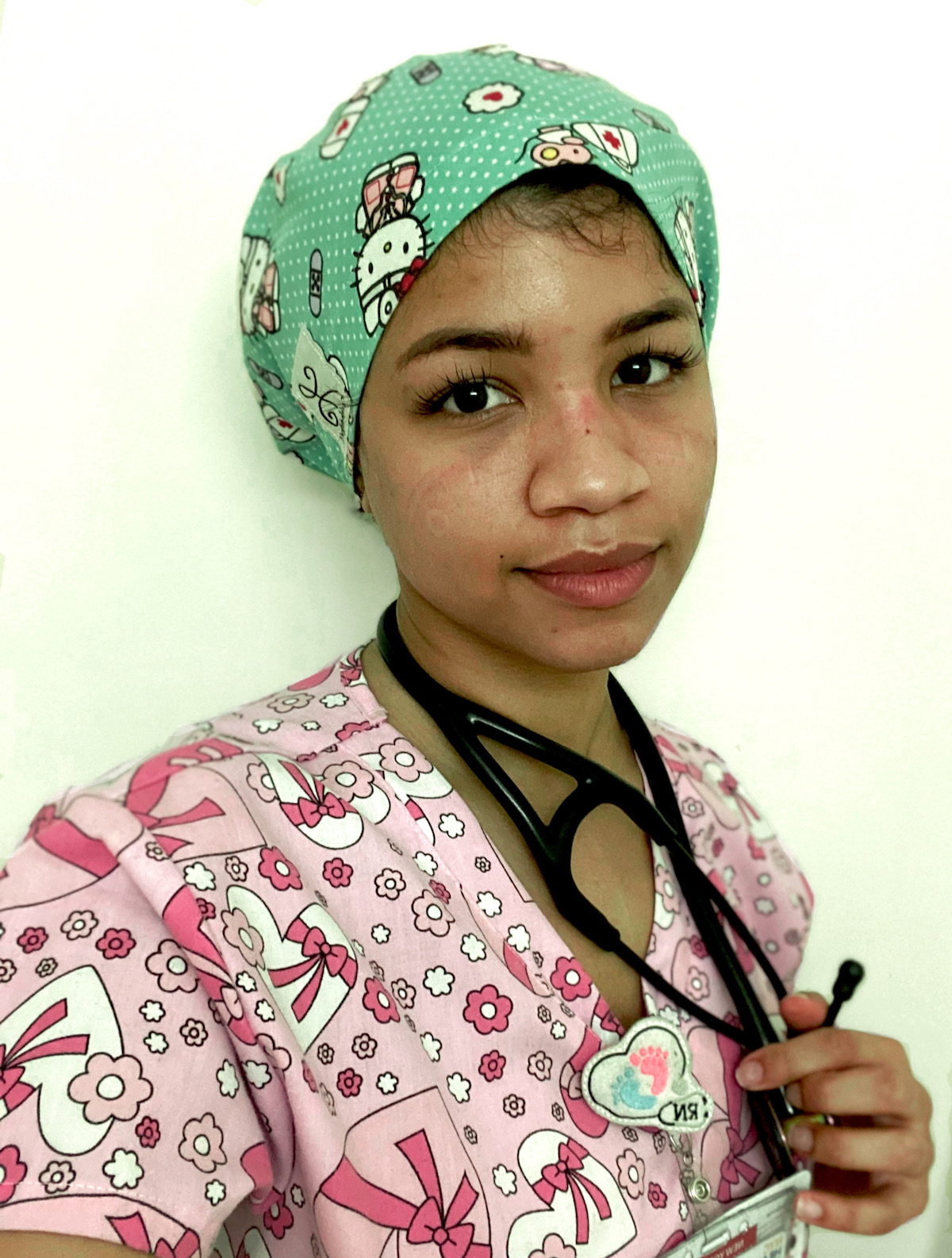
These are trying times for all citizens, but especially taxing on healthcare professionals around the world. We spoke to Angélica Ortiz, a Postpartum nurse from the Bronx, New York, to find out more about work and life inside hospitals at the epicentre of the pandemic.
Hey Angélica, can you tell us a little bit about yourself?
Angélica: Hey YEOJA Mag! I am a 26-year-old Postpartum nurse. I graduated nursing school last summer and was hired late September of last year. I am married to my high school sweetheart, going on 8 years now. I’m Dominican and currently reside in the Bronx. I used to love spending my days off cooking, going out with friends, or visiting family. Nowadays, I spend them at home, mentally preparing to go back to work.
What made you want to go into medicine?
Angélica: I didn’t have a magical moment of realization when it came to choosing my field. Growing up, I loved the sciences and felt the subject was the only one I was truly good at and understood. My mother was a nurse back in our country and my older sister eventually got into healthcare, so it was a natural profession for me and the only thing I could see myself doing when it came to choosing a career. I always felt I would be an asset in the mission of helping others and it came naturally to me to use my resources to help others become better.
This pandemic is something that even the most seasoned health care professionals are experiencing for the first time. As a newly graduated nurse (summer 2019), what has it been like to be thrust into the frontlines?
Angélica: It’s interesting to be asked this question because it seems sometimes that those around me expect me to handle this pandemic with confidence and bravery, but often I feel afraid and unsure of what my role is in all of it. I was only off orientation for about a month and was already struggling to find some stability, while also fortifying my skills and learning how to function on my own. Once the pandemic took off here in New York, it kind of spun everything around and ever since, it’s been a game of trying to catch up to the policies and procedures that seem to change almost daily.
Seeing mothers who test positive separated from their newborns has been heartbreaking. They are alone and away from their families since visitors are not allowed now. The nurses are overwhelmed and unable to give them the care and attention they need during those crucial first days as mothers. It’s been rough.
It is still very hard for many people to grasp the severity of COVID-19, especially when life for some seems unchanged. Yet the reality is that 10.022 people in New York City alone (as of 20 April 2020) have lost their lives to COVID-19. It seems as though one of the causes of this is that the sick cannot be visited. This means only those who have lost loved ones or are working inside hospitals are seeing how dire the day-to-day situation currently is. CNN recently visited SUNY Downstate to show viewers just how dire the situation inside hospitals in New York City truly is. Where are you currently working, and can you tell us more about what day-to-day life is like for nurses and doctors fighting COVID-19?
Angélica: I am currently working in the Mother-Baby unit in one of New York’s city Hospitals (I’d rather not say the name due to policies in place.) Day to day life is exhausting. We are facing something we do not have enough research on yet and [loads of] patients are coming in. I can’t speak for ICU and med-surg nurses who are caring for actively dying or critically ill patients; I can only speak for those in the maternal-child field.
Trying to bring security and reassurance to our patients while we ourselves are afraid is difficult. Working with mothers whose results come back two days after testing means we are all very exposed to the virus. Patients are currently treated as negative until proven otherwise, so we are aware that we may be exposing not only ourselves, but the other patients under our care who may test negative while we await the results. However, with the lack of supplies and staffing, we cannot afford to gown up for all patients while their results are pending.
What does a “regular” shift currently look like for you?
Angélica: When I arrive at the hospital, my temperature is tested before entry. Then, I make the line to the elevator waiting area, since more than 20 people are not allowed to wait at once. I arrive on the unit and quickly gather my supplies and take report. Anxiety runs high as we all prepare for the day, having some confirmed cases and most patients pending results. We have travel nurses on our unit, sent to handle Covid-19 patients while the “house” nurses deal with the rest. However, at any given moment during the day, it may be that one or more of the patients under our care has test results come back positive.
Luckily, our census has been lower, since we have been discharging quicker than usual and our sister unit Labor and Delivery hasn’t had a high amount of births. However, at any moment, Labor and Delivery can fill up and we’ll receive a wave of patients. Complications with the mother or newborn may also delay discharge. We are a unit without private rooms, so moms that are positive and need isolation take up two beds at once, while babies are placed in one room in isolettes. We don’t have enough rooms for what is coming.
Currently, many meetings and phone calls are taking place to attempt to address the issue of not having enough space. During a regular shift, without a clerk and many times a technician, we are also doing duties such as answering phones, handling all the paperwork, and fetching supplies for the unit and our patients. Fetching supplies is harder now, sometimes we have to leave the unit and pick up supplies ourselves, as opposed to having them delivered.
A regular day consists of almost non-stop work. Teamwork is really what gets many of us through the day and out the door.
“Trying to bring security and reassurance to our patients while we ourselves are afraid is difficult.”
If you could get one message across to citizens around the world, what would it be? If you could get one message across the President of the United States right now, what would it be?
Angélica: To the citizens of the world, I’d say: please be careful and stay home. It is easy to dissociate from what is happening without close ones suffering from the virus or without watching any news. This virus is real and it is changing our lives and the way we practice by the minute.
To the president, I’d say I am disappointed in the lack of severity this received and also the lack of a proper response to this issue. It often feels like we are left to fend for ourselves with little to no resources while those in government cover up the deficiencies in our healthcare system to protect their image. Our healthcare system has been flawed for a long time now and it is only being highlighted now. A lot of the issues we are facing are not new.
Healthcare professionals have their own personal lives and relationships outside of work. How has being on the frontlines of this battle impacted your personal life and relationships?
Angélica: Yes, yes, and yes, we healthcare workers are human beings and have families and lives outside of our jobs. Being on the frontlines has completely impacted my life outside of work. I have not seen my parents in over a month for fear of spreading the virus to them. I used to visit them just about every week. Lately, I started setting up Zoom meetings where my parents can talk to me and my two older sisters and our families. This helps us keep in touch so that we know everyone is okay.
I also miss my friends, although I appreciate the daily support and encouragement; they text me every day. I miss simply getting a hug and grabbing brunch [with them]. Many of them text me the difficulties their families are facing and those they have lost, which makes me sad, but we can join together in prayers and at least grieve together through calls.
As far as my husband is concerned, he remains my only source of support. He’s my best friend and has tested positive for the virus. He’s currently on sick leave and at home, so it’s been nice seeing him more often. He’s also a first responder and, on the daily, we don’t get to see each other very much. Sometimes the hardest part of my job, especially as a fairly new nurse, has been facing all these challenges alone.
“This virus is real and it is changing our lives and the way we practice by the minute.”
Who do you live with, and how do you ensure that they stay safe? How do they help you get through this period emotionally?
Angélica: I live with my husband, a police officer. When the virus first came, we both knew at some point, we’d both contract it since we have high levels of exposure. Despite that, we try to ensure our safety by washing our uniforms in bleach, wiping down everything we touch, and showering from head to toe as soon as we arrive home. It’s been helpful for me that we are both in [similar] fields since we face many of the same issues. We also do not have children (yet!), so there is significantly less fear than for some others. To get through this period emotionally, we both remain very open in our communication. We write each other notes in our lunches and hear each other vent about our days – sometimes for hours – when we are finally together.
This is a stressful time for everyone but undoubtedly more stressful for health care professionals who are not only physically and mentally exhausted from longer work hours and the volume of patients being seen, but also exhausted from the pain of being around death. How do you cope?
Angélica: Due to my specialty, I am not around death firsthand. I commend the nurses who are working with actively dying patients and reach out to my friends in those fields as much as I can.
We at mother-baby deal more with the emotional aspect of the separation between families during the process and recovery from birth, which is exhausting on its own. We also have absolutely no idea how the virus is affecting our littlest patients, so we fear when babies sneeze too often or seem kind of jittery it may be the beginning of symptoms. We also often hear over the intercom the codes for those who are dying.
Lately at my hospital, the song “Don’t Stop Believing” has started playing throughout the entire hospital whenever someone is extubated or discharged home after surviving from covid-19. This helps us all find hope, hearing the song up to 15 times in one day sometimes. Although the days when we hear it less can be gloomy. I cope by journaling and talking to my husband.
On particularly hard shifts, if I feel the need to cry, I’ll take a minute and go to the bathroom and FaceTime my husband, who gives me a little motivational speech in one minute to get me back out there. Most often though, there isn’t much time to focus on our own exhaustion. Our concern for our patients and the effects of short-staffing on the rest of our teams keep us coming back.
“Lately at my hospital, the song ‘Don’t Stop Believing’ has started playing throughout the entire hospital whenever someone is extubated or discharged home after surviving from covid-19. This helps us all find hope, hearing the song up to 15 times in one day sometimes.”
What can everyday citizens do to support health care professionals in their community? What do governments need to do to support health care professionals?
Angélica: Everyday citizens, please stay home. There are still so many people outdoors not social distancing. If you MUST go out, educate yourselves on hand hygiene the proper use of masks, social distancing, and minimize the time you spend out there.
Continue reaching out to your healthcare worker friends – the tremendous support I’ve received online has really helped me keep going. Sometimes the simple “thank you” from a stranger matters more to me than I can express.
Also, educate your families and friends on what you learn. Share information to keep each other safe. To all the citizens who have dedicated their talents, such as art and sewing masks, in support of healthcare workers, keep going. We see you and appreciate you. Governments need to take a closer look at ways to fix our broken healthcare system. We need more staffing, more supplies, and funding. Not only now, during this pandemic, but always.

In the US, COVID-19 is disproportionately impacting black Americans and yet although the media has called attention to this fact, very little is being said about the true reasons (systemic and institutionalized racism that puts black Americans at a disadvantage on multiple fronts). What kind of changes do we need to see happening in the healthcare sector to mitigate these effects? (i.e. universal healthcare, fair medical treatment for all levels of income)
Angélica: We need to see so many changes in the healthcare system to level the playing field for black Americans. The media will always fail to highlight the issues with racism we face here in America. In the healthcare sector, fair medical treatment and more culturally competent care are definitely necessary. It is not a problem I think universal healthcare would even solve, as long as the system itself is pitted against black Americans.
I have witnessed unfair treatment for my own patients, [and am] sometimes forced to advocate for them. I am very grateful for my head nurse – a black woman herself – who helps us correct many unfair situations. Sometimes this includes helping our darker-skinned mothers in situations where they face more obstacles in their discharge and keeping their children. However, facing these issues in one of the most diverse hospitals in the world, a city hospital where we serve the most underserved populations, really makes me worry about other environments [that are not as sensitive to the needs of black Americans]. It is not highlighted nearly enough that black Americans do not receive fair treatment within the medical field.
Despite all of this, we hope there is some light peeking through the end of this very long tunnel. Even through times of extreme pain and adversity, human beings are resilient and are able to come together. Can you share with us what the camaraderie has been like between nurses, doctors, and janitors, and how you continue to support each other and find love for what you do each day?
Angélica: The camaraderie has been tremendous during these times. On the regular, my coworkers are the reason I make it through the day. With the pandemic, I don’t know what I’d do without them. We join in prayer before every shift and do our best to help each other, even carrying out tasks for patients that are not assigned to us to help another [coworker] who may be swamped.
Those working in nutrition work closely with us and do not hesitate to switch to disposable trays when one of our mothers test positive; our janitors do not hesitate to gown up and go into rooms when requested. Everyone has kind of put on the “it has to be done” attitude during this time; we don’t complain anymore. On a personal level, we text each other, often asking how we’re doing on supplies, asking how we’re coping, and telling each other to stay safe. It’s been nice to feel that sense of teamwork. It really takes a huge team of people to get us through this time.
_
*Statistics as of 20 April 2020
Photographs curtesy of Angélica Ortiz. For more coverage on the Corona Pandemic, click here.